The Essential Role of Data in Healthcare: Managing the COVID-19 Crisis and Recovery
We hear every day from virtually every one of our hospital customers and prospects that “If it’s not COVID related, we’re not doing it.”
This is an understandable response when confronted by a crisis like we have never seen before. Healthcare providers are seeing massive decreases in revenue as they suspend elective procedures and routine office visits to reduce risks of COVID-19 exposure and redeploy resources to respond to the crisis. They are simultaneously experiencing dramatic reductions in emergency visits as even patients with acute conditions stay away from hospitals out of fear of being exposed to the virus.
However, experience is showing that analytics and insights from data are essential to responding to the immediate COVID crisis. They are also critical for managing our way through the next 12 to 18 months as hospitals seek to resume some semblance of normal operations to meet their community’s health needs while also responding to the peaks and valleys of COVID-19 cases that will inevitably recur.
I recently had the opportunity to chat with Mike Ross, VP of Analytics and Population Health for OhioHealth, about this very subject as part of a webinar hosted by Healthcare Innovation. We discussed how the data management capabilities OhioHealth deployed allowed them to handle the immediate COVID-19 crisis and look to create a new, financially sustainable operating model moving forward.
Data-Driven Executive Decision-Making Requires Reliable, Trustworthy Data
According to Ross, OhioHealth leadership is using the insights gained from data as a key input into their decision-making. Early on in their response, they established a command center staffed with senior executives who were supported by analytic dashboards.
Before the pandemic, OhioHealth had developed a holistic enterprise data strategy that was well into implementation. This provided a solid data management foundation that supported their efforts to both respond to the immediate crisis as well as approach reopening their health system to elective and more normal operations.
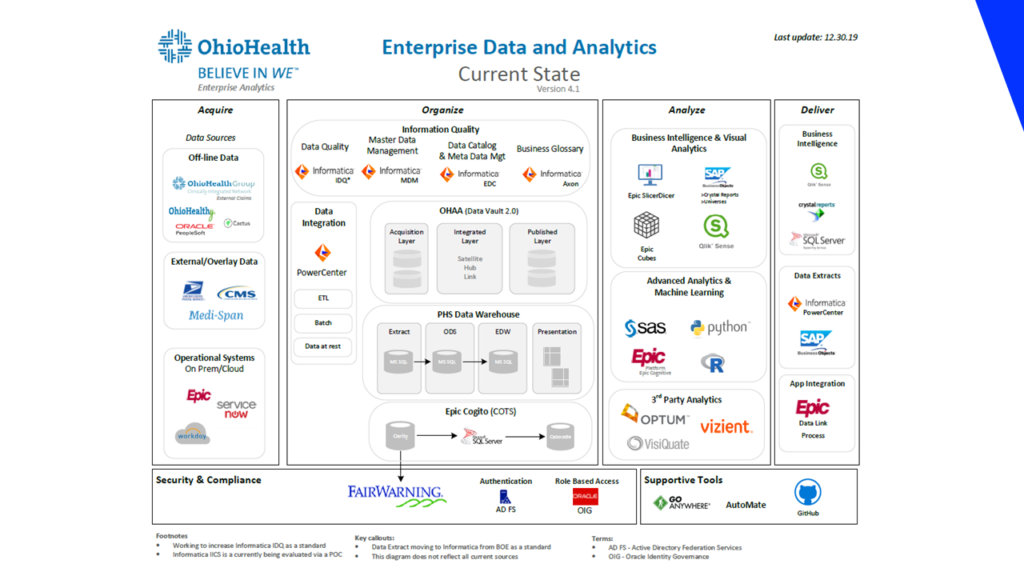
Epic serves a central role in the data strategy—with analytics as a key competency. The end goal of the strategy was the digital transformation of the health system, driven by data and analytics. But beyond being particularly well thought-out and delivering value to the enterprise, by Ross’ own description there is nothing particularly unique about the approach and architecture.
Once the pandemic hit, “We found very quickly things that were nice to know became not as important as the things we had to know,” says Ross. This ability to rapidly prioritize the most important deliverable and build a functioning solution in a small number of days was a common theme throughout our discussion.
Another common theme was that the trustworthiness of the data was never questioned by executive leadership. Ross attributes this trust to the organization’s investment in a proper data architecture.
Reliable, Trustworthy Data Requires Holistic Data Governance
Overnight, the COVID-19 crisis created an insatiable demand for analytics and access to trustworthy data. OhioHealth was able to accelerate their data governance program by three months, the formation of a data science team by six months, and the community of practice for self-service business intelligence by two years, thanks to having the right strategy and technology components in place.
OhioHealth sees themselves as operating in two parallel crises—and in fact they have two separate command centers: A COVID-19 command center; and a command center based on becoming a new, financially viable organization, with the goal of getting back non-COVID patients and re-instating elective procedures. The ability to run predictive models forecasting demand, staffing levels, resource utilization and other key measures is essential in effectively allocating resources to COVID patients and knowing what capacity is available for elective procedures.
Master Data Management Is Foundational for Digital Patient Engagement
But having the capacity to take care of routine patients visits and elective procedures is only part of the challenge. Where before the crisis OhioHealth was often challenged with meeting patient demand for services, reopening and rescheduling elective visits and procedures required a very different type of engagement with patients and their families.
In many cases people were reluctant to return to the hospital, for varied and often very personal reasons. This required a disciplined and focused patient engagement strategy using master data management capabilities that not only delivered information to patients and their families, but also captured their preferences for how they liked to communicate (email, text, phone, etc.) and exhibited knowledge of prior interactions (whether the patient had already declined rescheduling an elective surgery, for instance). This patient engagement is increasingly digital and more personalized as a matter of necessity as OhioHealth works to reengage with their community and resume more normal operations.
Unanticipated effects of the pandemic that will be critical moving forward include the need to get deep into the supply chain. As citizens on the street, we saw almost daily news coverage citing the shortage of personal protective equipment, ventilators, and other essential medical supplies. These issues brought the supply chain into acute focus and is an area of future investment for OhioHealth.
Predictive Analytics Takes Center-Stage
Next-generation analytics has been a hot area for innovation over the past few years; however, all too often we hear our healthcare provider customers say, “We can’t even do basic reporting right now, so we’ll worry about that fancy stuff later.”
The COVID-19 crisis has brought into clear focus what is meant by predictive analytics and why it is so invaluable in responding to a crisis. Under normal circumstances, health systems are accustomed to working at capacity; longstanding experience and “rules of thumb” have been adequate predictors of future demand. But with the COVID-19 crisis, there is no historical basis or experience to use for planning.
In this situation, predictive models become essential for executive decision-making and planning. This is the case at OhioHealth, where a small team of four data scientist were in the center of the storm for building models and informing executive decision-making—albeit with the stark admission that the models were wrong, but would get better over time with more data and more real-world experience.
The importance of reliable and trustworthy data to support building these models cannot be overstated. We’ve all heard the rule-of-thumb that data scientists spend 80% of their time finding and preparing data (fixing data quality issues and the like) and only 20% of their time gaining insights from the data. In a crisis and with only a precious few data scientist, this is the last thing you want as an executive. You want the data to be available, findable, and trustworthy and your data scientists spending 80% (or more!) of their time building and refining models to provide the mission-critical insights to guide executive decision-making.
Next Steps
Ross and I conclude our discussion on OhioHealth’s data strategy with his key takeaways. I’m not going to be a spoiler and recount them here—listen to the webinar to get the full benefit of his insights.








